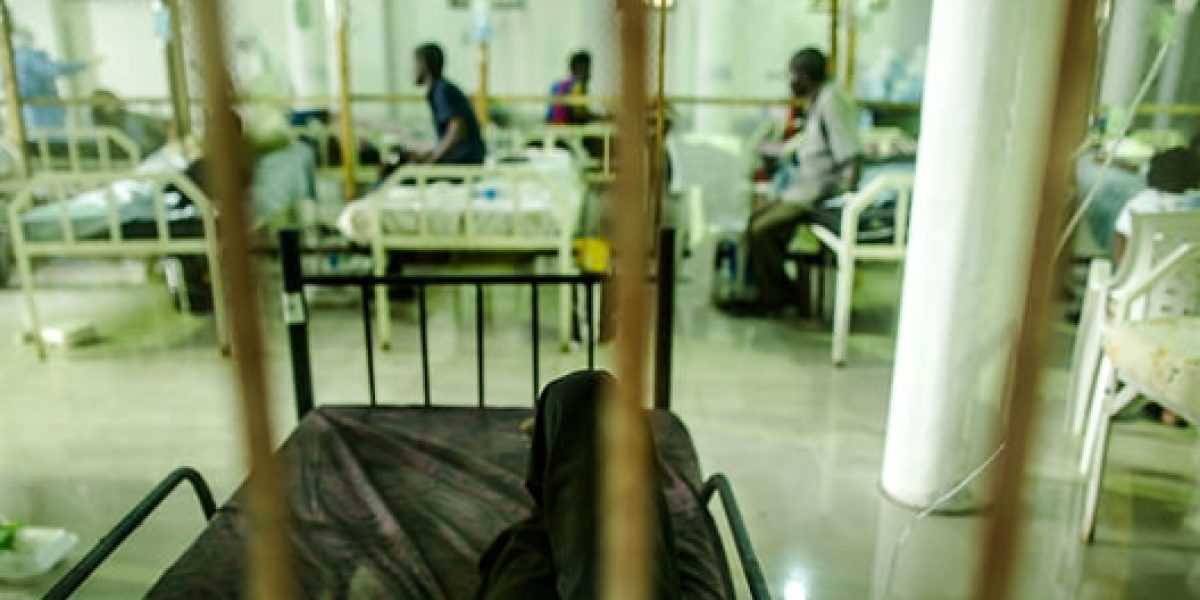
The initial cases of this outbreak were reportedly from the forested region in southeastern Guinea in Gueckedou prefecture, close to the borders of Liberia and Sierra Leone. The virus has spread to Sierra Leone, Liberia, Nigeria, Senegal, with an additional reported case in the United States.
In September 2014, the UN Security Council (UNSC) declared Ebola a threat to peace and security, during its first emergency meeting on a public health crisis. Secretary General Ban-Ki Moon also announced the deployment of a new UN emergency health mission, the UN Mission for Ebola Emergency Response (UNMEER). UNMEER has five priorities: stopping the outbreak, treating the infected, providing essential services, preserving stability, and preventing further outbreaks.
Containing the spread of Ebola is made increasingly difficult because of the delayed public health response to the disease, a lack of infrastructure within the affected countries, and increasing travel restrictions on travellers from these countries. Independent health advisors to the World Health Organization (WHO) have advised against isolating these states, but fear of the disease spreading makes this increasingly difficult to enforce.
The Ebola crisis has highlighted the ineffectiveness of existing health institutions in Africa, drawing attention to the need for a revised longer-term strategy on the continent, especially with regard to international health diplomacy approaches. The following brief considers the Western and Chinese approaches to the Ebola outbreak, their long-term strategies on the continent, while considering how these contrasts reflect the differences in Western and Chinese diplomatic engagement on the continent more generally. Considering the merits and gaps of both horizontal and vertical healthcare approaches, this brief argues that international health diplomacy should place greater emphasis on building horizontal, integrated healthcare systems to avoid similar pandemics like that of Ebola.
Responses to the Ebola Outbreak
The Ebola virus has prompted debate around effective intervention, vertical and horizontal interventions, and the longer-term effectiveness of Chinese versus Western interventions in Africa.
Both China and the West have taken similar short-term approaches to the Ebola emergency. China has sent a fifty-nine-member laboratory team to West Africa to help contain the epidemic. Provision of human resources is essential, as there are limited local resources in the region. The team will boost the presence of the 115 medical experts in West Africa. China has also sent millions of dollars in medical supplies. The Unites States’ and Western response mechanisms have included millions of dollars of humanitarian aid, clinic support, and doctors sent to West Africa, as well as military personnel and treatment centres.
The Western approach to healthcare in Africa has focused heavily on vertical targeting of disease, meaning concentrated attention on the disease itself, eradicating the spread of the disease, or provision of services to curtail the effects of the disease, as identified in the UNMEER mission objectives. China’s approach to healthcare in Africa has traditionally been a strictly horizontal, integrated system method, which focuses instead on the development of access to medicines, hospitals, and infrastructure. Historically there has been a contrast in the effectiveness of a vertical versus horizontal approach.
In light of the Ebola epidemic and considering longer term sustainability of healthcare systems, it would appear that China’s long-term ‘horizontal’ strategy, if adopted throughout Africa, would provide greater advantages to African healthcare. Providing assistance to build up the infrastructure to maintain a horizontal healthcare system will help increase developing states’ ability to fight disease outbreaks initially, and in the case of Ebola, would have been instrumental in stemming the spread of the disease. Acknowledging this fact, the Ebola Response Roadmap outlined by the World Health Organization members (China and the US included), included a detailed approach to containing the spread of the virus that specified both an (arguably vertical) emergency response, as well as emphasising the importance of providing for sustained horizontal mechanisms for the near future.
Vertical and Horizontal Systems
The two dominant healthcare approaches are vertical and horizontal (or integrated) systems of engagement. Both systems have been questioned as to their effectiveness in developing countries.
On the one hand, vertical systems target specific health issues with interventions that are not fully integrated into health systems. Vertical systems of healthcare have been successful in eradicating smallpox and reducing death and morbidity from vaccine-preventable diseases. Yet vertical programs have limited integration with general healthcare, which has led to replication of efforts in certain countries, inefficient healthcare delivery, and fragmented health systems, as the disease-specific focus neglects the need for integrated development of healthcare systems, establishment of healthcare infrastructure, and grassroots expansion of sustainable healthcare environments.
The vertical systems model of healthcare has been identified as one of the root causes of the failure to eradicate malaria, which poses a consistent problem throughout Sub-Saharan Africa. The Ebola-stricken countries are also prime examples of how a lack of solid healthcare infrastructure can diminish the capacity of states to contain disease outbreaks.
Vertical systems also potentially divert human and financial resources from resource-constrained health systems. Vertical programs are, however, attractive to donors and political bodies, as results are quick and such systems are easier to manage than horizontal programs. Despite the weaknesses attributed to vertical programs—which arise due to a lack of follow-through for active case surveillance, integration of disease surveillance into primary healthcare services, and specific disease response services—funding from sources like the Global Fund and Gavi, the Vaccine Alliance, has targeted vertical programs in health systems. The Global Fund and Gavi, despite having differing approaches, have had success in slowing the rate of HIV infection, tuberculosis, and malaria (Global Fund) and providing vaccines and immunisation against diseases such as pneumococcal disease and meningitis worldwide (Gavi).
Horizontal approaches are delivered through publicly financed healthcare systems, also referred to as comprehensive primary care. Horizontal approaches, which include the financed provision of routine immunisation, community directed treatment strategies (for example, the control programs for African onchocerciasis, also known as river blindness, or Robles disease) focus on prevention and care for prevailing health problems.
Horizontal systems are cost effective and sustainable in the long term, can deliver preventive services to poorer people who can’t afford private healthcare, and are preferential for policymakers, because of the appeal of long-term sustainability. In addition, if financed by government revenue and a broader, sustainable health plan, horizontal healthcare systems can be integrated into the public sector. However, such care systems only work effectively in stable environments, which most developing states lack due to poor infrastructure and limited resources. And more often than not, resource deficient countries cannot afford to implement integrated programs into public healthcare systems. As a result, international health assistance programs have tended to rely on vertical short-term approaches, despite evidence that horizontal care could offer a more effective integrated and comprehensive health care solution in the long term.
An ideal healthcare response would combine vertical and horizontal health systems, particularly in countries with weakened post-war economies such as Liberia, Sierra Leone, and Guinea. Such an approach would also seek to distribute health assistance funding to improve the conditions necessary for long-term sustainable healthcare solutions to be instituted. To this end, the WHO has called for coordination between both horizontal and vertical health approaches to strengthen existing health systems and ensure successful communicable disease response programs.
Parallels with Economic Engagement in Africa
What is interesting to note, beyond the need for collaborative and cooperative healthcare management in this instance, is how each power, acting autonomously, has provided different systems of healthcare in developing nations.
As one of Africa’s primary investment champions, particularly in Sierra Leone, Liberia, and Guinea, China has a lot of economic investment at stake on the continent and much to gain from investment in healthcare in Africa. China’s health diplomacy in the Ebola outbreak, for instance, is strategic, in that China is building a hydroelectric plant in Guinea and has investment interests in West Africa. And China has been criticised for limited humanitarian involvement in the past, seeking only to assist where Chinese assets are threatened.
China has traditionally sought to build infrastructure and healthcare systems and invest in the continent, without interfering in a country’s governance, debt repayments, or political instability. This approach has drawn criticism from the West, as there is less concern for the human rights abuses taking place in these countries. China’s aim, however, is to develop Chinese resources and markets, with limited political and social interference in their target countries.
Comparisons can be drawn between health and political and economic diplomacy in Africa. Chinese investment in African business and infrastructure follows the same path as its health diplomacy. China’s Africa strategy focuses on multilateral diplomacy and a culture of vigorous international participation, particularly regarding health interventions. The Western approach has focused on facilitative, prescriptive strategies to enable democratic and economic reforms in developing states, in exchange for multilateral assistance.
The challenge with China is that it is still classified as a developing country and is still a recipient of development assistance. China has shouldered a lot of international responsibility and continues to make investments in Africa, but at the risk of its own citizens, including exposure of its own medical staff to the Ebola virus. The Beijing Consensus provides an alternative to Western-centred political and economic development reforms embodied in the World Bank and International Monetary Fund’s Washington Consensus. China steadfastly respects the internal sovereignty of states, despite poor governance and largely opaque political systems, without imposing reforms, such as those demanded by the West. Beijing’s soft power—friendly ties with Africa and provision of ‘no strings attached’ aid to political elites and those in need—is a far more attractive alternative to rigorous reform.
Western aid still outweighs Chinese humanitarian assistance, however, and there is a greater proliferation of Western donor-funded social development programs. This draws interesting parallels between styles of governance and economic assistance in this regard. This raises the question: should multilateral powers work to implement and integrate both vertical and horizontal systems, or should individual countries pursue their own agendas within Africa?
Recommendations
While the unwillingness of the Chinese to acknowledge political abuse of power in many African states poses a diplomatic dilemma, the Chinese health and investment approach in Africa—as opposed to highly vertical programmatic approaches—may be the most effective option in the long run. That being said, global powers have not collectively acted swiftly enough to the Ebola outbreak, necessitating the need for an instant vertical response to containing the disease.
The international community, including both Western and Chinese health diplomats, need to work together to find sustainable healthcare solutions to prevent such a disaster from occurring again. To that end, a number of recommendations can be made to facilitate these processes.
First, regular Security Council meetings should be held on public health issues in developing countries as a preventative diplomatic measure to ensure threats from communicable diseases are addressed before they become too large to manage at a national and regional level.
Second, to better integrate vertical and horizontal systems, better use needs to be made of potentially available workforces in countries, and promotion of workforce growth, in the form of contributions by the private sector, government incentives to engage the private sector, and standardisation of quality and service procedures is essential in attaining this goal.
Most important, regular policy, planning, and political cooperation are also needed from national governments, to make effective connections between health systems and workforces in countries. Combining vertical interventions and horizontal systems requires planning to deploy supply and personnel.
Finally, efforts should be made to broaden the skill sets of health workers to enable response to all interventions.
These strategies may be difficult to implement in developing countries, but with the correct support and combined systemic approach to healthcare, these challenges can be met and healthcare systems strengthened over time. This may also require increased dialogue between China and the West, possibly through joint healthcare investment plans, regardless of political differences.